-
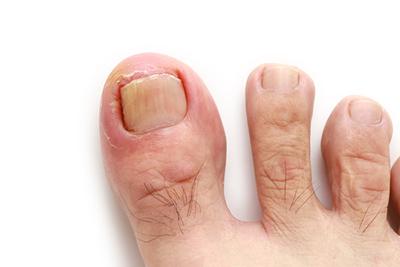
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.

-
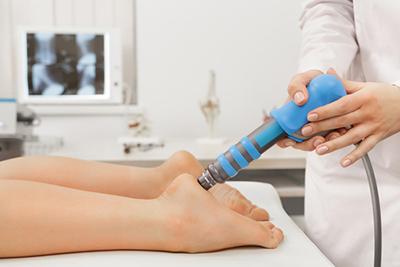
Managing Your Heel Pain
posted: Mar. 01, 2024.
-
What You Need To Know About Ingrown Toenails
posted: Feb. 01, 2024.
-
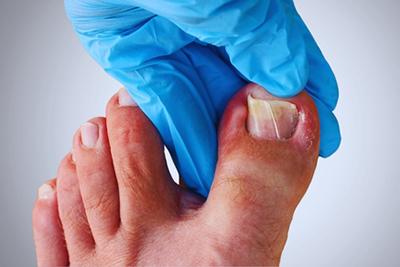
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
posted: Jan. 01, 2024.

-
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
posted: Dec. 01, 2023.

-
The Benefits Of Orthotics
posted: Nov. 01, 2023.

-
The Importance of Diabetic Care
posted: Oct. 01, 2023.

-
Bunion Treatment Options
posted: Sep. 01, 2023.

-
Foot Health for Children
posted: Aug. 01, 2023.

-
Diabetes and Foot Care: Tips for Maintaining Healthy Feet
posted: Jul. 01, 2023.

-
What You Need To Know About Taking Care of Your Feet
posted: Jun. 01, 2023.

-
Foot Conditions That Affect Athletes and How to Prevent Them
posted: May 01, 2023.

-
Common Causes of Foot Pain
posted: Apr. 01, 2023.

-
The Importance of Foot Care for Diabetics
posted: Mar. 06, 2023.
-
Benefits of Having a Podiatrist
posted: Feb. 01, 2023.


