-
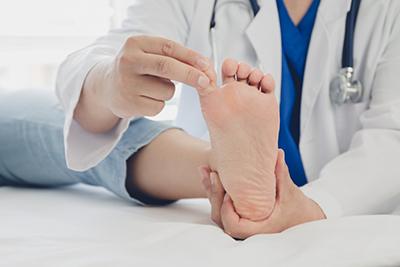
The Importance of Proper Footcare for Diabetic Patients
posted: Jan. 01, 2023.

-
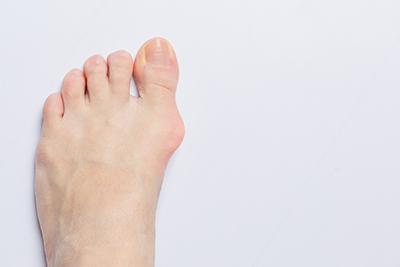
What Are Bunions and How Can They Be Treated?
posted: Dec. 01, 2022.
-
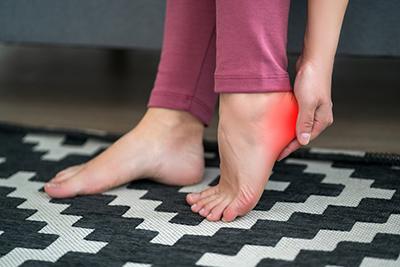
Causes of Heel Pain
posted: Nov. 01, 2022.
-
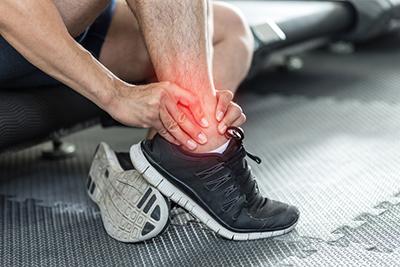
What To Do for Ankle Pain
posted: Oct. 01, 2022.
-
Is My Toe Broken?
posted: Sep. 01, 2022.

-
Are You Dealing With Bunion Pain?
posted: Aug. 01, 2022.
-
Ways To Prevent Ingrown Toenails and When To Seek Help
posted: Jun. 29, 2022.
-
Don’t Let Ankle Pain Slow You Down
posted: Jun. 03, 2022.

-
Treating Your Heel Pain
posted: May 05, 2022.

-
Treating Your Bunions
posted: Apr. 01, 2022.

-
Proactive Foot Care For Athletes
posted: Mar. 02, 2022.

-
What Are Fallen Arches?
posted: Feb. 01, 2022.
-
Arthritis and Your Feet
posted: Jan. 03, 2022.

-
Should I Get Custom Orthotics?
posted: Dec. 02, 2021.

-
Splinters in Your Feet
posted: Nov. 01, 2021.


